Back Health
It is estimated that 80% of people experience back pain at some point in their lives.
Back pain can be managed and future suffering can be reduced or avoided by using specific physical activity and lifestyle strategies.
At BeMoore Pilates, Yoga & Personal Training we offer the following services to help empower you to manage your symptoms and reduce future episodes:
Classes
Once a week is recommended as a minimum requirement (which can be combined as part of a home exercise program). 2-3 times a week is highly recommended. If your back pain has been diagnosed as non-specific- it is most likely you will be able to go straight into classes.
Private coaching may be recommended on a case-by-case basis.
Private coaching
If a pathology or nerve damage has been diagnosed we would highly recommend at least one private session before starting exercise. Some positions can exacerbate back pain, therefore it is imperative for us to examine you closely and offer alternatives if necessary.
Everybody is different, private training is recommended to design a solution bespoke to your body and needs.
Treatments for Back Pain
I would advise a multidisciplinary approach to back pain. Assist with behavioral, lifestyle, physical, nutritional (particularly overeating and intolerances), and physiological factors to help manage the current condition, and reduce the chance of further damage and future episodes.
Short-term: Many approaches might be recommended such as heat, massage, osteopathy, and physiotherapy, these may be necessary at the time but they are short-term fixes and need to be supported by longer-term changes.
Long-term: Lifestyle changes such as adapting to work environments, exercise, physical and mental patterning, and diet are long-term changes we may need to make to manage back pain for life.
Medication: Pain relief such as paracetamol and ibuprofen is often the only treatment sought by those in the acute phase. However, the GP may prescribe stronger pain relief such as codeine, or muscle relaxants such as diazepam if necessary.
Hot/cold: Many people benefit from the use of ice or heat packs to reduce pain and improve movement.
Stay active: Gone are the days of prescribing bed rest. Current thinking is that people who stay more active will recover sooner.
Avoid painful activities: If pain limits movement in the early days, then activities should be modified to avoid pain. However, people should appreciate that an element of discomfort is to be expected.
Physiotherapy: treatment may include hands-on manual therapy techniques such as joint mobilization, soft tissue massage, acupuncture, and exercise therapy.
Expert advice: Advice will be given about activity modification, posture, sleeping position, and movement to help people carry out their daily tasks as best as they can.
What are the specific risks of participating in exercise for clients with chronic non-specific low back Pain?
Providing that pathologies and nerve damage have been ruled out the risks of participating in the exercise are very low.
One should be mindful of the side effects of any medication and keep an eye out for any red flags.
If pathologies or nerve damage exist, I recommend at least one private session before starting classes, some people may need 6 -12 sessions to become confident in movement, everyone is different.
What are the guidelines and current best practice for back pain?
Always make sure you are exercising in a safe environment to the level that is suitable for you with a fitness professional that is trained in the area of care you require (back pain, pre-natal, post-natal, orthopedic conditions).
Always encourage feedback to your teacher if something does not feel right for you so they can advise as required or give you an alternative.
Varied movements in multiple directions are favorable for back pain patients.
Any exercise prescription should include many exercises that will develop fitness without undue pressure on the spine such as Pilates, Yoga, walking, and cycling.
A general aim of exercise for patients who are suffering from lower back pain is to increase exercise tolerance and prevent debilitation which is often caused by inactivity.
Special considerations according to ACSM –
- Trunk coordination, strengthening, and endurance exercises can be used to reduce low back pain and disability in individuals with subacute and chronic low back pain with movement coordination impairments. However, there is insufficient evidence for any benefits of single-dimension therapies such as abdominal strengthening.
- Response to back pain can be improved by providing assurance, encouraging activity, and emphasizing that more than 90% of low back pain resolves without specific therapies.
- There is a lack of agreement on the definition, components, and assessment techniques connected to core stability. The majority of tests used to assess core stability have not demonstrated viability.
- Abdominal bracing should be used with extreme caution because it increases spinal compression.
- Certain positions may aggravate LBP, most commonly flexion, extension or rotation. Find out which for each person and encourage movement at a reduced range in the mentioned direction.
- Certain individuals may experience a spread of pain in the lower limbs. Limits should be placed on exercises or activities that cause the spread.
- Flexibility exercises are generally encouraged. Hip and lower limb flexibility should be promoted.
- Consider progressive low-intensity aerobic exercises for those with chronic LBP with generalised pain and moderate-high for those with chronic back pain without generalised pain.
What are the red flags that would indicate that physical activity or specific types of exercise may be contraindicated?
Red Flags
These red flags would indicate an emergency referral (if not already diagnosed):
Red flags include:
- Mode of onset:
- Road traffic accident
- Major trauma
- Severe symptoms with sudden onset for example bilateral leg weakness or unremitting pain
- Suspected fracture or bony abnormality
History suggestive of tumour, carcinoma, infection:
- Over 50, under 20
- History of carcinoma
- Sudden unexplained weight loss
- Frequent urinary tract infections
- Drug abuse or HIV
- Recent fever
- Persistent night pain
- Loss of appetite
- Unusual lumps or growths
- Sudden fatigue
Cauda equina symptoms:
- Bladder disturbance, increased frequency or urinary retention
- Bowel or bladder incontinence
- Saddle anaesthesia, numbness in the saddle region
- Bilateral weakness or paraesthesia in the lower limbs
If you are currently experiencing a back pain episode and you begin to notice any red flags, I would recommend contacting a medical professional immediately.
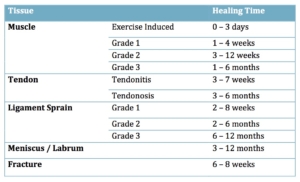
Healing Time Frames
The course of lower back pain
The course of lower back pain can consist of up to three phases.
- The acute phase -lasting for less than six weeks
- The sub-acute phase –lasting for between six and twelve weeks
- The chronic phase -lasting longer than twelve weeks
Approximately 90% of people are expected to become pain-free or have a dramatic reduction in symptoms, during the acute phase and in most cases, symptoms will resolve in around six weeks.
Only 10% will continue into the chronic phase.
Understanding Tissue Healing Time
Expectations have a huge effect on the mental and therefore physical health of a person. It is therefore healthy to have the knowledge and realistic expectations for healing timeframes.
Understand other factors that affect healing
Similarly to the factors that increase the risk of back pain, many of those will also slow down the rate of healing, for example. –
- lack of physical fitness /physical inactivity
- smoking and medication
- obesity
- stress and depression
- physical trauma
- awkward positions at work, frequent bending, and twisting, bad movement techniques, poor posture etc all increase the likelihood of reoccurring episodes and slow recovery.
- Pregnancy
- Poor nutrition
- Poor hydration
Activities
Activities
- Pilates, Yoga, lifting, Swimming, Dance
- Flexibility
- Muscular Strength and Endurance
- Cardiorespiratory Fitness
Find an activity/ies that work for you and your body, that you enjoy, and aim to have a balanced approach to strength, flexibility, and relaxation.
Back Pain is often something we may have to manage long-term and therefore finding an activity that is enjoyable to the individual is incredibly important. We also know how our mental health affects our back and the vicious circle of mental health/physical health and this heightens the importance of this further.
Positive reinforcement and the Nocebo effect
Keep language positive
There have been studies showing that if people are told something will hurt, they are more likely to experience pain – the nocebo effect.
Positive reinforcement and the nocebo effect.
A nocebo effect is said to occur when negative expectations cause the treatment to have a more negative effect than it otherwise would have.
Consider these statements –
- Your knees must be above your ankle to protect your knee
- If you don’t engage your core you will hurt your back
- Engaging your glutes (in the shoulder bridge) compresses your lower back
- There is only one way of performing a pose
Consider words like stabilize instead of protect
“Do your best”, or “Listen to your body” instead of “stop if it hurts”
What is back pain?
Low back pain is pain, muscle tension, or stiffness localized below the rib margin and above the inferior gluteal fold.
Back Pain can be non-specific or as a result of an injury or a condition.
How common is low back pain?
Low back pain is very common; it is estimated 4 out of 5 adults will suffer low back pain at some point in their lives.
94% will have non-specific back pain where there is no underlying disease or pathology.
The number of people with back pain increases with age, starting in school and peaking in adults of 35 – 55 years; back pain is also common in adolescence as well as adults.
After an initial episode of low back pain, 44 – 78% of people have relapse symptoms. While 26 – 37% relapse in the form of absence from work.
High-pressure sedentary management roles increase risk, as do jobs involving heavy manual labor- especially those involving repetitive lifting and twisting.
Evidence suggested that low back pain should not be considered temporary and consequently neglected since the condition presents with a period of attacks and temporary remissions. It is therefore important to implement strategies to reduce the chance of reoccurrence.
Evidence also shows that 90% of people with low back pain stop consulting healthcare professionals within 3 months. Yet, most will still be suffering one year after their initial consultations.
It is more common in women (the risk for a woman increases with each pregnancy) than in men.
What is non-specific low back pain?
Non-specific lower back pain is also called mechanical back pain and although it’s very difficult to diagnose an exact cause, it will involve structures in the lower back such as the ligaments, muscles, and tendons, the joints between the vertebrae, and the intervertebral discs.
The cause may vary between spinal ligaments, strained muscles, muscle spasms, facet joints, or disk irritation- the origin is mechanical and practically unidentifiable.
Not having a “cause” or “diagnosis” can be incredibly frustrating for the individual with non-specific lower back pain, but thankfully it can usually be reduced, treated, and kept at bay by maintaining a good posture, lengthening muscles that need to be lengthened and strengthening those that are weak.
Our mental and emotional health is just as important to take care of as well as our physical health. Back pain episodes have been known to be triggered by emotional trauma. Increasing our ability to manage stressors, counseling, therapy, meditation, and breathwork may also be a consideration for our healing and maintenance program.
Non-specific lower back pain is the most common, accounting for 94% of cases.
What is back pain with nerve root pain / radicular pain?
This includes sciatica and other pain where the nerve impinges, typically as it exits the intervertebral foramen- potentially by a herniated intervertebral disk or the piriformis muscle as it passes through the pelvis.
These are fairly uncommon and account for around 5% of low back pain cases.
Although they are fairly uncommon, Fitness Professionals might come across Sciatica more often, especially as Pilates Teachers.
What is a spinal pathology?
There are a number of different forms of spinal pathology including:
- Osteoarthritis
- Rheumatoid Arthritis
- Ankylosing Spondylitis
- Bone disorders
- Fractures
- Infections
- Tumors that can all cause low back pain
These causes are low and account for less than 1% of low back pain cases.
To learn more about supporting you/your client with a spinal pathology please request to join our Level 2 Back Pain Course
What reduces the risk of back pain?
It is wise to have a multidisciplinary approach to back pain and look at behavioral, lifestyle, physical, nutritional and physiological factors to help reduce the chance of further damage and future episodes.
Some of the below risks are non-modifiable but the rest can be changed or managed to reduce the risk of back pain:
- lack of physical fitness /physical inactivity
- smoking and medication
- obesity
- stress and depression
- physical trauma
- awkward positions at work
- frequent bending and twisting
- heavy or repetitive lifting
- Lifting or carrying heavy loads and movements involving twisting and overreaching
- jarring, gripping, vibration, or repetitive actions
- prolonged sitting and or standing
- mechanical loading (ie children that carry a bag of more than 20% of their body weight have high LPB rates)
- Bad technique: Bending awkwardly or pushing or pulling incorrectly.
- Poor posture, especially in sustained positions such as slouching in a chair, sitting at work, and when driving.
- functional movement and alignment
- Pregnancy (non-modifiable)
- number of children (non-modifiable)
- major scoliosis (non-modifiable)
- increased age (non-modifiable)
Activity: write a list of the modifiable factors that are contributing to the back pain and for each factor create short and long-term goals/ steps to improve these factors.
How do our brains effect the development and management of back pain?
Stress, Anxiety, and Depression
Stress over a long period of time suppresses the immune system function, creates endocrine (hormonal imbalances), and can increase musculoskeletal tension. Body positions that are associated with fear include spinal flexion (hunched shoulders or curling into a ball) removing the lordotic curve of the spine.
In addition, whilst the body experiences stress it diverts blood away from the muscles and away from the gut which increases muscle tone as part of the flight or fight response. This is advantageous as far as physical activity is concerned. However, in many modern situations, the body is sitting inactive- so the additional blood flow and tension can lead to spasms and tightness.
Many people are not even aware that they are/have been experiencing stress, anxiety, or depression. For some, it has become a way of life and they may have experienced this from a very young age. Sometimes acknowledging the presence of stress, anxiety, or depression can be the hardest but most freeing step.
Even if the stress has not been long-term, the fact that the individual has been walking around in pain and it has affected their life is bound to have created some stress on the body. It can be a primary or secondary
It can become a vicious circle of stress = back pain = stress = back pain = depression = back pain = anxiety…..
It is therefore incredibly important to reduce or manage the influence of stress on our bodies.
Stress Management techniques include –
- Cognitive Behavioural Therapy
- Meditation
- Breathwork
- Feelings and Needs Coaching
Fear of Movement
In my experience ‘Fear of movement” is one of the greatest reasons for prolonged injury / reduced recovery.
Avoidance of normal activities out of fear of worsening pain is the natural instinct to protect a body part.
A better understanding of pain means we now know that pain is a function of the central nervous system. Although initially triggered by peripheral nociceptors, after this acute incidence the pain exists in the nervous system and is not being caused by trauma to tissues. Understanding this and gently beginning to move in a normal way, helps the body to realize that it is safe to move and stop sending the pain signals.
If movement is avoided out of fear this prevents the body from relearning natural movement and reinforces the pain pathways, which can make recovery much slower.
The Nocebo Effect
Many people know the placebo effect. The Nocebo effect describes the phenomenon of experiencing an unfavorable effect from an inert stimulus. Nocere comes from the Latin to hurt, harm or damage. Nocebo means ‘I will hurt”, ‘I will harm”, ‘I will damage”. The effect can occur not just from the ingestion of a pill, but even from the suggestion of it.
If people are told something will hurt, they are more likely to experience pain. The same would be if they believe it will hurt it is more likely to. This can also introduce anticipatory anxiety which triggers the activation of cholecystokinin, a hormone that facilitates pain transmission.
Avoid using fear-based language with yourself/ your clients. Focus on the positives and what to do rather than what not to do where possible.
Catastrophising
Associated with the all-or-nothing way of thinking. Some people are more prone to thinking this way and making generalizations. They may think of the worst-case scenarios and limit their activities to what they think a person with back pain ‘should’ and shouldn’t do. Often this is based on inaccurate beliefs and involve them protecting themselves from pain by avoiding certain movement.
Negative expectations and beliefs
Having a pessimistic or negative outlook often occurs alongside catastrophizing and is known to reduce the impact of treatment interventions. The relationship between body and mind is so strong that emotions and beliefs have a physiological influence on the body. Thankfully the reverse is also true!
Learning to observe, challenge and better understand our thoughts and the patterns of the mind can be very helpful in this case.
Cognitive Behavioural Therapy and bespoke Meditation can be very helpful in this case.
How does inactivity v’s activity affect Back Pain?
Inactive
When we become inactive, some muscles become tight and some become weak. This means that the body can not support itself as it should and our posture begins to change. Pressure on the body can create, discomfort, and injury.
Inactivity can also be linked to feeling down, or even depression. The more inactive we are, the more down we feel and then it becomes a vicious circle. We have to work hard to break the cycle. Committing ourselves to regular classes or sessions can help to break this cycle.
Being Active
“Safe” movement has been proven to reduce pain levels.
By strengthening the areas that have become weak and stretching (lengthening) the areas that have become tight we can reduce the pressure on the lumbar, reducing pain and the chance of further damage and future episodes.
Increasing the blood flow and nutrients to the soft tissues in the back improves the healing process and reduces stiffness.
Working on bringing the posture back or maintaining posture will help to prevent further injury.
Sciatica, Disk Herniations and Piriformis Syndrome
Sciatica
The name sciatica relates to any nerve pain originating in the lower back and radiating into the buttock, back of the thigh, and even as far as the calf and foot.
Location
Signs and symptoms
Signs and Symptoms of sciatica can vary in nature and severity.
Pain may be felt from the lower back, down the back of the thigh and lower limb to as far down as the foot, depending on where the sciatic nerve is being compressed.
Leg pain symptoms will normally affect only one side of the body with the leg pain being worse than any back pain.
Buttock pain is usually worse on sitting and clients may experience a sharp, shooting pain which is more noticeable when standing up.
Sensations Some clients may experience tingling, “pins and needles”, a burning sensation, or numbness along the course of the nerve.
Difficulty moving Some clients experience weakness or a feeling of heaviness in the affected leg or foot, making it difficult to move.
Causes of Sciatica
Causes of Sciatica
Symptoms of sciatica occur when the sciatic nerve root is irritated or compressed as it exits the spine between L3 and L4. This is most commonly due to a herniated or ‘slipped disc, or less commonly when the sciatic nerve itself is compressed.
Other than a herniated disc, irritation or compression may be due to degenerative disc disease, spinal stenosis, spondylolisthesis, and piriformis syndrome.
Clients experiencing any of the symptoms of sciatica should be checked out by a medical practitioner. They may be able to determine the cause of the symptoms by taking a thorough client history and performing a number of physical tests.
Treatment of Sciatica
Treatment of Sciatica
- Conservative treatment aims to reduce inflammation and irritation of the nerve. This may be achieved through-steroidal anti-inflammatory drugs (NSAIDs) such as Ibuprofen, and over-the-counter pain relief such as Paracetamol. Stronger pain relief and muscle relaxants may be prescribed by a GP if necessary.
- Physiotherapy may include exercise therapy to manage symptoms and stretch and strengthen the lower back, this will often be similar to the entry levels of Pilates.
- Exercise programs may also be followed if recommended by the GP by a qualified exercise professional.
- Cognitive behavioral therapy may also be used to help clients manage pain and remain positive.
- If conservative treatment is unsuccessful then surgery may be required. Surgical options include: Discectomy, Laminectomy, Spinal fusion
Disc Herniations
Disc Herniations
Signs and symptoms of herniation can vary greatly depending on its area and size. If there is no pressure against the nerves, as might be the case in the initial degenerative stage, then there may be localised aching or pain or no pain at all.
If there is pressure against a nerve, depending on where the disc is herniated there may be pins and needles, electric shock-type pain, numbness or weakness in the arms or legs.
Disc herniations most commonly occur between the fourth and fifth lumbar vertebrae and the fifth lumbar and first sacral vertebrae as this is the area of the spine that takes most of the body weight.
Treatment of herniation will depend on the severity of the symptoms.
Rest – Initially clients will be advised to rest from aggravating activities, such as prolonged sitting, bending, lifting and reaching. Symptoms generally settle within a few days as the protrusion retreats.
Medication – Medication may be required such as NSAIDs or paracetamol. The GP may prescribe stronger pain relief such as codeine if the pain is severe. Muscle relaxants such as Diazepam may also be prescribed in cases with severe muscle spasms and stiffness.
Discectomy – If the symptoms are severe or long-lasting a discectomy may be performed to remove the section of the disc that is bulging.
Exercise – If the pain is severe, complete rest may be required initially. However, once symptoms have settled people are encouraged to keep moving and perform gentle exercises. Physiotherapy treatment and exercise programming can help relieve symptoms.
Exercises for sciatica caused by disk herniation
You can discuss with your client the exercises to avoid, those that will help centralize the symptoms, and those you would recommend as symptoms settle.
Stage 1 –
Exercises to avoid until your client’s symptoms have resolved include exercises involving flexion such as –
- Roll Down
- Spine Stretch
- Saw
- Roll Up
- and any version of rolling including Rolling Back, Crab, Seal, Open Leg Rocker
Exercises that centralize symptoms include exercises encouraging lumbar extension for example
- Half or Full Cobra
- Cat Stretch in extension only
Stage 2 –
As symptoms settle centralize the emphasis is on strengthening the core and lower back muscles and stretching tight structures with exercises such as:
- Swan Dive
- Swimming
- Single then double knee folds
- Shoulder Bridge
- Pelvic tilts to gently stretch and mobilize the lower back, as long as they do not exacerbate symptoms
- Gluteal and hamstring stretches
Piriformis Syndrome
Piriformis Syndrome
Piriformis syndrome is the name given to conditions involving the piriformis muscle. In a very small number of people, the sciatic nerve passes through the piriformis rather than underneath it on its course through the pelvis. The sciatic nerve can be impinged by the piriformis muscle and the piriformis muscle itself can be strained.
Sciatica symptoms such as pain and tingling in the buttock and radiating down the leg can be caused if the sciatic nerve is compressed by the piriformis. The piriformis may be strained due to tightening or shortening of the muscle as a result of trauma or overuse. The symptoms in this instance tend to be deep aching in the buttock aggravated by sitting or walking upstairs.
Treatment generally includes stretching exercises for the piriformis and other tight muscles such as the gluteals and hamstrings. A physiotherapist may also use soft tissue techniques such as massage and stretching.
The main consideration of exercises for piriformis syndrome is to stretch the piriformis muscle to relieve pain along the sciatic nerve. There are a number of ways to stretch the piriformis including:
- Prone lying glute stretch
- Supine glute stretch
- Supine lying opposite knee to chest and shoulder
Spinal Stenosis
Spinal Stenosis
The most common cause of spinal stenosis is wear-and-tear changes in the spine related to arthritis.
Exercises for sciatica caused by spinal stenosis are those that encourage opening the passageway through which the spinal cord passes, thereby relieving impingement or irritation.
These exercises focus on stretching the lower back extensors and strengthening the spine flexors.
Suitable exercises include:
- Child’s Pose
- Knees to Chest Stretch
- Cat Stretch in flexion
- Curl Ups
Pilates exercises such as –
- The Hundred
- One Leg Stretch
- Double Leg Stretch
- Scissors
- Roll Up
To learn more about supporting you/your client with any of the causes of Sciatica please request to join our Level 2 Back Pain Course
Key areas to note according to the ACSM
Having researched guidelines from all over the world the ACSM (American College of Sports Medicine) gave what we believed to be the most up-to-date advice.
- LBP is not a serious or life-threatening medical condition.
- Most episodes will improve.
- A negative mindset, fear avoidance behavior, negative recovery experience, and poor pain coping behaviors are more strongly associated with persistent pain than tissue damage.
- Scans do not determine the prognosis of the current episode or improve clinical outcomes.
- Graduated exercise and movement of the spine in all directions are safe and healthy for the spine
- A weak core does not cause LBP. Many over-tense their back and while it’s important to keep the trunk muscles strong it is also helpful to learn how to switch them off.
- Pain flare-ups are more related to changes in activity stress and mood rather than structural damage.
- Effective care for LBP can be relatively cheap and safe. This includes patient-centered education, fostering a positive mindset, and optimizing physical and mental health, including exercise, social activities, healthy sleeping habits, achieving healthy body weight, and having a purpose.
I would personally like to comment on note 1.
Although it might not be classed as “serious” or life-threatening”, having experienced back pain myself I know all too well how challenging, exhausting, and frustrating it can be to live with back pain. These notes are not to invalidate anyone’s pain, discomfort, or reduction in quality of life but to share the current guidelines for exercise professionals.
Other areas to discuss
Hypermobility
People with Hypermobility may take longer to heal.
Find out more about Hypermobility
Request to join a training on Hypermobility
Flexibility Training
Taught correctly this can be a more accessible way of fraining Flexibility than a practice like Vinyasa Yoga.
Often in Yoga, we come across transitions, extension, flexion, or rotation that irritates Back Bain.
Find out more about Flexibility Training
Request to join a training on Flexibility Training
Training Habits
Training at 70 – 80% v’s 100/110% will yield the same flexibility results and will cause less degradation (pain and soreness) than stretching at 100/110 %.
Recovery
Create an optimum recovery environment –
- Rest
- Get enough sleep
- Activate the parasympathetic nervous system to encourage the body to go into a recovery state.
- Optimise your nutrition
- Stay hydrated
- Use FAR infrared therapy if accessible.
- Heat has been proven to be very successful in reducing back pain.
Knowledge Check
Knowledge Check
- What % of people with back pain have what we call ‘non-specific”, or “mechanical back pain’?
- What is “non-specific” back pain?
- What is Sciatica?
- Name a Spinal Pathology.
- List 3 things we can do to reduce the risk of back pain.
- How can stress affect back pain?
- How can “Fear of movement” affect back pain?
- What is “The Nocebo Effect”?
- How does activity affect back pain?
- Which sort of approach should we take toward treating back pain?
- Providing that pathologies and nerve damage have been ruled out what are the risks of participating in the exercise for those with back pain?
- List a Red Flag
- What is a Red Flag?
- What is a Par-Q?
- What are the time frames for tissues to heal?
- Name another factor that will slow down the healing process.
Some References
Courses
Future Fit Pilates Training for Orthopedic Conditions
Active IQ L4 Diploma in Lower Back Pain
Premier Global Personal Training
Dylan Werner – One Movement 300-hour Advanced Training (Flexibility Training, Advanced Anatomy, Breathwork, and Meditation)
Cognitive Behavioural Therapy Diploma
Mindfulness Diploma
Books
The Physiology of Yoga – Andrew McGonigle
Anatomy Trains – Thomas Myers
ACSM’s Guidelines for Exercise Testing and Prescription